Squamous cell carcinoma
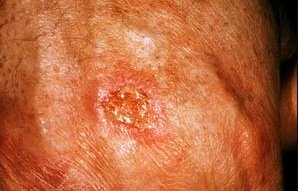
Squamous cell carcinoma arises in the squamous cells that make up most of the skin's upper layers (the epidermis).
These carcinomas may occur on all areas of the body, including the mucous membranes and genitals, but are most commonly found in the following areas frequently exposed to the sun:
- the outer rim of the ear
- the lower lip
- anywhere on the face
- bald scalp
- even beneath a full head of hair on your scalp
- neck area,
- hands - both palm and back
- arms
- legs
Squamous cell carcinoma: the basics

Think of a squamous cell carcinoma (SCC) as a skin cancer that is a type of tumor affecting the skin.
The main thing to be observant of, is when you notice any change on the surface of your skin as they will occur when cells in the skin change.
These happen most often where the skin has been exposed to UV rays, whether from the sun or otherwise, as well as where you may have incurred some sort of injury or have inflammation.
This type of skin cancer is at least twice as frequent in men as in women.
They rarely appear before age 50 and are most often seen in individuals in their 70s.
The earliest form of this carcinoma is known as either "squamous cell carcinoma in situ" or Bowen's disease. This is when the cancer tumor has not yet invaded any of the surrounding skin tissue.
You will see it as a large reddish patch, often bigger than an inch, or 2.5 cms, with a scaly or crusty feel.
This is actually quite similar to actinic keratosis, which is a precancerous skin lesion that can turn into a SCC, although this is not known to be a common event.
Squamous cell carcinoma: causes

Sunlight.
Excessive exposure to sunlight is the most prevalent cause of these carcinomas.
Tanning Beds.
However, the frequent use of tanning beds also increases the risk of SCC.
People who use tanning beds are 2.5 times more likely to develop this carcinoma than those who don't.
Skin injuries
These are another important risk factor as the cancer can occur in burns, scars, ulcers, persistent sores and even areas exposed to X-rays or chemicals such as arsenic or petroleum by-products.
Inflammation.
Sometimes if you have a bad infection with skin inflammation a carcinoma can appear.
Weak immune system.
Anything that causes the immune system to weaken makes it harder for your natural system to defend itself. HIV and other immune deficiency diseases, chemotherapy, anti-rejection drugs used in organ transplantation, and even excessive sun exposure itself all weaken the immune system, making it harder to fight off disease and thus increasing the risk of SCC and other skin cancers.
Inheritance?
Occasionally, these carcinomas arise spontaneously on what appears to be normal, healthy skin. Some researchers believe the tendency to develop these cancers can be inherited.
Risk Factors for squamous cell carcinoma
The following risks for squamous cell skin cancer are what you should be aware of:
- Type one skin type - light-colored skin, blue or green or gray eyes, or blond or red hair
- Regular daily exposure to UV rays without protection. eg outdoor workers, suntan-worshippers
- Having acquired serious sun burns in years past, especially if at a young age
- Getting older and your immune system becoming less resilient
- Having had a large number of x-rays
- Toxic chemical exposure through factory work, farming pesticides, environmental toxic exposure, etc
- Anyone with an inherited, highly UV-sensitive condition such as xeroderma pigmentosum
NB: Though naturally dark-skinned people are less likely than fair-skinned people to get skin cancer, it is still essential for them to practice sun protection.
Can squamous cell carcinoma metastasize?
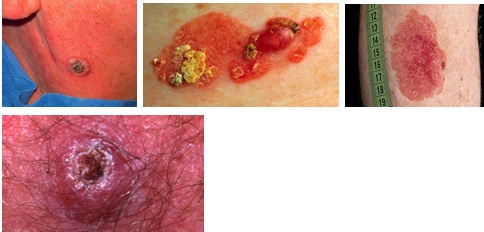
More than 700,000 new cases of squamous cell carcinoma are diagnosed every year in the United States alone.
That makes it the second most common skin cancer, after basal cell carcinoma.
A SCC is capable of spreading much faster than a basal cell carcinoma. However, it is still relatively slow-growing.
Rarely, it will spread (metastasize) to other locations, including internal organs, but according to the Skin Cancer Foundation, squamous cell cancers are actually the cause of about 2,500 deaths per year in the US.
Squamous cell carcinoma: what to look out for?
Unfortunately when people check their skin for signs of skin cancer they don't easily recognize them - the telltale spots are really so commonplace.
According to Dr Roger Ceilley, MD, FAAD, Clinical Professor, Department of Dermatology, University of Iowa, the warning signs for both SCC and BCC include:
- A spot, sore, shiny bump or nodule, scaly lesion, or wart-like growth that continues to itch, hurt, crust, scab, erode, ooze, or bleed. These often look like warts
- An open sore or wound that does not heal within 2-3 weeks
- A white, yellow, or waxy scar-like area, or a reddish patch or irritated area
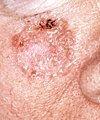 A persistent, scaly red patch with irregular borders that sometimes crusts or bleeds
A persistent, scaly red patch with irregular borders that sometimes crusts or bleeds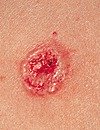 An elevated growth with a central depression that occasionally bleeds. A growth of this type may rapidly increase in size
An elevated growth with a central depression that occasionally bleeds. A growth of this type may rapidly increase in size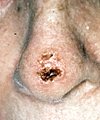 An open sore that bleeds and crusts and persists for weeks
An open sore that bleeds and crusts and persists for weeks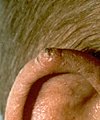 A wart-like growth that crusts and occasionally bleeds
A wart-like growth that crusts and occasionally bleedsSquamous cell carcinoma: main symptom
The main symptom of the existence of a squamous cell carcinoma problem is a growing bump that may have a rough, scaly surface and flat reddish patches.
Typically this bump occurs on the face, ears, neck, hands, or arms, or anywhere exposed to UV rays. But of course, they may actually occur anywhere else on the body.
Squamous cell carcinoma: What if I detect something?
Squamous cell carcinomas detected at an early stage and removed promptly are almost always curable and cause minimal damage.
As part of a regular check-up, your doctor or dermatologist will assess your skin and look at the size, shape, color, and texture of any suspicious areas.
If he agrees with you that skin cancer is a possibility, a piece of skin tissue will be removed from the area and examined under a microscope. This is called a skin biopsy. This biopsy must be done to confirm the diagnosis of squamous cell carcinoma or any of the other skin cancers.
There are many types of skin biopsies and the exact procedure will depend on the location of the suspected skin cancer. If tumor cells are detected, treatment is then required.
If left untreated, squamous cell carcinomas will eventually penetrate the underlying tissues and even become disfiguring. A small percentage even metastasize to other tissues and internal organs and then become fatal. Most common metastases arise on areas of chronic inflammatory skin conditions as well as on the ear, nose, lip, and mucosal regions, which include the mouth, nostrils, genitals, anus, and the lining of the internal organs. Not pleasant at all!
Therefore, any suspicious growth you have should be followed up with a visit to your physician or dermatologist without delay.
About 95% of these tumors can be cured if they are removed or treated in good time. The trick is to catch them early and not ignore the warnings.
After removal, new tumors may develop though, so it is important to keep checking regularly.
Squamous cell carcinoma: Treatment
The choice of treatment will be based on the type, size, location, and depth of penetration of the squamous cell tumor, as well as the age and general condition of health.
Treatment is usually done with a local anesthetic in a physician's rooms where pain and/or discomfort is minimal and there is rarely any pain afterwards.
The following treatment options are available (as listed by the Skin Cancer Foundation):
- Mohs Micrographic Surgery
Using a scalpel or curette (a sharp, ring-shaped instrument), the physician removes the visible tumor with a very thin layer of tissue around it.
This layer is immediately checked under a microscope thoroughly.
If tumor is still present in the depths or peripheries of this surrounding tissue, the procedure is repeated until the last layer viewed under the microscope is tumor-free.
Mohs saves the greatest amount of healthy tissue, appears to reduce the rate of local recurrence, and has the highest overall cure rate about 94.99 percent of any treatment for squamous cell carcinoma.
It is frequently used on tumors that have recurred, are poorly demarcated, or are in hard-to-treat, critical areas around the eyes, nose, lips, and ears, as well as the neck, hands and feet. After removal of the skin cancer, the wound may be allowed to heal naturally or be reconstructed using plastic surgery methods. - Excisional Surgery
The physician uses a scalpel to remove the entire growth, along with a surrounding border of apparently normal skin as a safety margin.
The wound around the surgical site is then closed with sutures (stitches).
The excised tissue is then sent to the laboratory for microscopic examination to verify that all cancerous cells have been removed.
The accepted cure rate for primary tumors with this technique is about 92 percent.
This rate drops to 77 percent for recurrent squamous cell carcinomas. - Curettage and Electrodesiccation (Electrosurgery)
The growth is scraped off with a curette, and burning heat produced by an electrocautery needle destroys residual tumor and controls bleeding.
This procedure is typically repeated a few times, a deeper layer of tissue being scraped and burned each time to help ensure that no tumor cells remain.
It can produce cure rates approaching those of surgical excision for superficially invasive squamous cell carcinomas without high-risk characteristics.
However, it is not considered as effective for more invasive, aggressive squamous cell carcinomas or those in high-risk or difficult sites, such as the eyelids, genitalia, lips and ears. - Cryosurgery
The physician destroys the tumor tissue by freezing it with liquid nitrogen, using a cotton-tipped applicator or spray device.
There is no cutting or bleeding, and no anesthesia is required.
The procedure may be repeated several times at the same session to help ensure destruction of all malignant cells.
The growth becomes crusted and scabbed, and usually falls off within weeks.
Redness, swelling, blistering and crusting can occur following treatment, and in dark-skinned patients, some pigment may be lost.
Inexpensive and easy to administer, cryosurgery may be the treatment of choice for patients with bleeding disorders or intolerance to anesthesia. However, it has a lower overall cure rate than the surgical methods.
Depending on the physician's expertise, the 5-year cure rate can be 95 percent or higher with selected, generally superficial squamous cell carcinoma. However, cryosurgery is not often used today for invasive squamous cell carcinoma because deeper portions of the tumor may be missed and because scar tissue at the cryotherapy site might obscure a recurrence. - Radiation
X-ray beams are directed at the tumor, with no need for cutting or anesthesia.
Destruction of the tumor usually requires a series of treatments, administered several times a week for one to four weeks, or sometimes daily for one month.
Cure rates range widely, from about 85 - 95 percent, and the technique can involve long-term cosmetic problems and radiation risks, as well as multiple visits.
For these reasons, this therapy is mainly used for tumors that are hard to treat surgically, as well as patients for whom surgery is not advised, such as the elderly or those in poor health. - Photodynamic Therapy (PDT)
PDT can be especially useful for growths on the face and scalp.
A photosensitizing agent, such as topical 5-aminolevulinic acid (5-ALA), is applied to the growths at the physician's office and it is taken up by the abnormal cells.
The next day, the patient returns, and those medicated areas are activated by a strong light. The treatment selectively destroys squamous cell carcinomas while causing minimal damage to surrounding normal tissue.
However, the treatment is not yet FDA-approved for squamous cell carcinoma, and while it may be effective with early, non-invasive tumors, overall recurrence rates vary considerably (from 0% - 52%), so the technique is not currently recommended for invasive squamous cell carcinoma.
Redness and swelling are common side effects.
After treatment, patients become locally photosensitive for 48 hours where the 5-ALA was applied, and must avoid the sun. - Laser Surgery
The skin's outer layer and variable amounts of deeper skin are removed using a carbon dioxide or erbium YAG laser.
This method is bloodless, and gives the physician good control over the depth of tissue removed.
It actually seals blood vessels as it cuts, making it useful for patients with bleeding disorders, and it is also sometimes used when other treatments have failed.
But the risks of scarring and pigment loss are slightly greater than with other techniques, and recurrence rates are similar to those of PDT.
This technique is also not yet FDA-approved for SCC. - Topical Medications 5-fluorouracil (5-FU) and imiquimod
Both FDA-approved for treatment of actinic keratoses and superficial basal cell carcinomas, are also being tested for the treatment of some superficial squamous cell carcinomas. Successful treatment of Bowen's disease, a noninvasive SCC, has been reported. However, invasive carcinomas should not be treated with 5-FU.
Some trials have shown that imiquimod may be effective with certain invasive SCC's, but it is not yet FDA-approved for this purpose.
Imiquimod stimulates the immune system to produce interferon, a chemical that attacks cancerous and precancerous cells.
Squamous Cell Carcinoma: After treatment care
Most treatment options will require cutting, so the aftercare of your skin is important if you wish to minimize the scarring.
In some cases, however, removal of a larger tumor will necessitate some reconstructive surgery that may involve a skin graft or flap.
In cases where a nose, lip or ear in involved, more extensive reconstructive surgery may be chosen.
In all cases, where any one squamous cell tumor has occurred, there is an increased chance for developing another, especially in the exact same area or nearby vicinity.
This happens usually within the first two years after the initial surgery so due diligence in aftercare for your skin is vitally important.
Should the carcinoma recur, a different type of treatment may be suggested. Mohs Micrographic Surgery is very efficient for recurrences.
References
- American Cancer Society. Cancer Facts and Figures 2006. Atlanta, GA: American Cancer Society; 2006. [PubMed]
- Basal cell and squamous cell cancers: NCCN Medical Practice Guidelines and Oncology:V.1.2009. Accessed July 15, 2009.
- Hexsel CL, Bangert SD, Hebert AA, et al. Current sunscreen issues: 2007 Food and Drug Administration sunscreen labeling recommendations and combination sunscreen/insect repellant products. J Am Acad Dermatol. 2008;59:316-323. [PubMed]
- Lautenschlager S, Wulf HC, Pittelkow MR. Photoprotection. The Lancet [Early online publication], May 3, 2007.
- Ridky TW. Nonmelanoma skin cancer. J Am Acad Dermatol. 2007;57:484-501. [PubMed]
- Wood GS, Gunkel J, Stewart D, et al. Nonmelanoma skin cancers: basal and squamous cell carcinomas. In: Abeloff MD, Armitage JO, Nierderhuber JE, Kastan MB, McKenna WG, eds. Abeloff's Clinical Oncology. 4th ed. Philadelphia, Pa: Churchill Livingstone;2008:chap 74.
- Skin Cancer Foundation



